Dementia risk doubled in people with high on this major personality trait.
Being neurotic may double the risk of developing dementia later in life, research reveals.
The major personality trait of neuroticism involves a tendency towards worry and moodiness.
People who are neurotic are more likely to experience negative emotions like depression, anxiety, guilt and envy.
However, the link between neuroticism and dementia only occured in people experiencing long-standing stress.
In other words, neurotic people are particularly sensitive to chronic stress.
Neurotic people not exposed to excessive stress were at no greater risk of dementia.
Dr Lena Johannsson, the study’s first author, said:
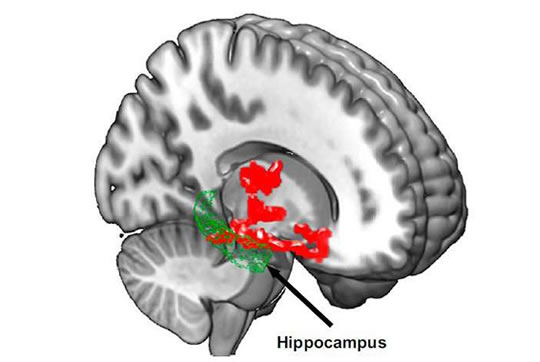
“We could see that the women who developed Alzheimer disease had more often been identified in the personality test 40 years earlier as having neurotic tendencies.
We found a clear statistical correlation for the women who had at the same time been subject to a long period of stress.”
The study followed 800 women with an average of 46 for almost four decades.
They were asked if they had experienced prolonged periods of stress.
This meant a month or more of ongoing stress related to family, work or health that created feelings of nervousness, fear and irritability.
Thirty-eight years later, one-in-five had developed dementia.
The risk was substantially higher, though, in those who were neurotic.
An even more vulnerable group were those who were both neurotic and introverted — women with this combination were at the highest risk.
Dr Johannsson said:
“We know that many factors influence the risk of developing dementia.
Our personality may determine behavior, lifestyle and how we react to stress, and in this way affect the risk of developing Alzheimer disease.”
However, neuroticism can be changed by therapy and its effects can be reduced.
Dr Johannsson said:
“Some studies have shown that long periods of stress can increase the risk of Alzheimer disease, and our main hypothesis is that it is the stress itself that is harmful.
A person with neurotic tendencies is more sensitive to stress than other people.”
The study was published in the journal Neurology (Johansson et al., 2014).